
MicroInjection of the Tecnis™ IOL
©2004. Robert M. Kershner, MD, MS, FACS
Boston, Massachusetts
By now most surgeons have either heard of the modified prolate anterior surface
IOL that neutralizes the eye’s spherical aberration (Tecnis™ Z-9001,
AMO, Inc.) or have already adopted it into their cataract practices. Despite
numerous studies demonstrating the Tecnis’ ability to improve visual acuity,
improve contrast perception, especially at night and at night when glare is
present1, and the FDA designating it for improved functional vision and safety2,
many surgeons have been slow to accept this new evolution in IOL optics.
Tecnis unfortunately got off to a slow start due at least in part to the absence
of a reliable injection system that would allow surgeons to implant the IOL
through a small incision. and have developed injection systems that take into
account the subtleties of injecting this lens optic. As a surgeon who has studied
the unique characteristics of this new technology IOL, I would like to share
my extensive experience with implanting the Tecnis IOL under a variety of circumstances.
AMO’s acquisition of Pfizer/Pharmacia Ophthalmics and the Tecnis brand,
has created a new opportunity to integrate AMO’s well known success with
IOL injection systems to a lens style that requires special attention with implantation.
The AMO Silver Series™ T Injection system has now been validated for the
Tecnis IOL. Combined with the Silver Series II cartridge, the marriage is complete.
Surgeons have a readily available and easy to use system to incorporate the
Tecnis technology into their armamentarium of IOLs. Because this IOL is not
your average spherical implant, the unique characteristics of the modified prolate
anterior surface and stiff PVDF haptics create special requirements when loading
and unloading the IOL into an injector and into the capsular bag.
The Tecnis IOL is a posterior chamber, 3-piece foldable IOL, with a CapC design
for posterior capsular bag fixation. The Z-9000 with a12.0mm overall length
and its counterpart, the Z-9001 with a 13.0mm overall length is made of a next
generation silicone, a UV-absorbing polysiloxane. The optic is biconvex, with
a patented modified prolate anterior surface, and a square optic edge with an
index of refraction of 1.46.
The two clear haptics, made from polyvinylidine fluoride are known for their
strength, but remain somewhat stiff during implantation. The haptics come off
the IOL optic at 900 takeoffs and are angulated 60. These characteristics
of the 911A platform from which they are derived are very important in assuring
proper centration as well as avoiding tilting of the IOL within the capsular
bag maximizing the potential for the optic to deliver its full benefit. They
are unfortunately, the same culprits that can make the loading, folding and
unfolding of the lens problematic.
Some surgeons in their previous early experience with this IOL, know what can
happen when the attention is not paid to the loading process, an inadvertent
haptic capture in the nosecone of the cartridge by the injector plunger can
crimp or bend a haptic, or worse yet, cause a complete destaking, taking a piece
of the IOL optic with it. This can fortunately be completely avoided when
the proper loading procedure is strictly followed.
The AMO Unfolder™ Silver Series T Injector reusable handle and Silver
Series II disposable single-use cartridge is similar to many presently in use
and is easy to use. Follow these simple tips to maximize successful implantations
of the lens. I have found that I can easily implant the Tecnis IOL through a
sub 3mm incision and routinely do not need to enlarge my standard 2.4mm clear
corneal incision. When you first start loading this lens it is best if the following
procedure is done under the operating microscope. Once comfortable with the
method, the lens can be loaded on the side table without magnification. I feel
that demonstrating the technique for your scrub assistant by using a video monitor
or by viewing through the operating microscope facilitates the learning process.
1. First remove the cartridge from its sterile packaging and place it on the
table so the nose cone faces to the left (at the 9 o’clock position).
You need not open the cartridge completely, in fact, a slight bend to the hinge
works best when positioning the IOL optic under the wings. It is easier to load
this lens with the cartridge on a table for stability, rather than trying to
hand hold the cartridge and the lens at the same time.
2. I suggest using a very small ribbon of an ophthalmic viscosurgical device
(OVD) such as Healon®, Healon GV®, Vitrax® or Healon 5®, on
the length of the hinge and sparingly into the troughs of the cartridge.
Avoid using dispersive agents such as methylcellulose which can result in inconsistent
lOL delivery and leave an undesirable coating on the optic. When using Healon5,
which is an excellent lubricant, recognize that it is quite viscous and can
actually compete with the IOL for space, so less is more, use it very sparingly
to get the same effect as with the less viscous agents. If you get a little
too generous with your OVD it can work against you. There is nothing worse than
an IOL covered with an OVD if you don’t get it positioned under the cartridge
wings on the first try (think: greased pig competition).
3. Remove the IOL container from its sterile package and place it flat on the
table. Press on the cover and remove it. Using blunt forceps gently slide one
of the blades into the groove overlying the right side haptic and lift out the
IOL (I prefer the modified prolate IOL lens holding forceps made for me by Rhein
Medical, Tampa, FL. It is specially designed to hold a non-symmetric optic without
slipping or damaging it).
4. With the cartridge tip pointed to the surgeon’s left, and 12 o’clock
being where the tip is, load the IOL approximately 0.5 mm to 1.0 mm behind the
IOL diagram shown on the cartridge wing. Position the leading haptic anchor
at the 3 o’clock position and the trailing haptic anchor at the 8 o’clock
position. Loading the IOL too far from the nosecone may not allow position of
the leading haptic. Loading it too close may prevent the trailing haptic from
remaining outside of the folded cartridge.
5. Before letting go of the lens, use the forceps blades to press the optic
under the edges of the two wings of the cartridge (with a little practice this
goes pretty easily, as your first attempt to load the lens is usually your best
shot).
6. With the forcep blades removed and slightly opened, position them flat onto
the surface of the lens optic to move the IOL back and forth along the edge
of hinge. This assures a tactile and visual check that the optics are secured
under the grooves of the cartridge wings. If they are not, reposition the lens
to make sure the IOL optic is captured under the cartridge wing edges. The resilience
of the optic material and the highly polished surface of the forcep blades reduces
the chance of inadvertent damage to the optic.
7. Next, while holding the optic into position to assure that it does not pop
out of the grooves, gently fold the cartridge wings. The IOL optic should have
a concave configuration and be well secured under the grooves of the cartridge
wings.
8. Manually position the leading haptic using the closed forceps tips under
direct visualization so that it is directed into the cartridge nosecone and
complete the closure of the cartridge.
9. Visually inspect that the trailing haptic remains out of the cartridge. If
the trailing haptic is trapped under the wing edge or bends toward the optic
give it a gentle sweep with the forcep’s blade. You need not reopen the
cartridge to do this.
10. Load the silicone tip onto the injector plunger.
11. Grasp the injector making sure the plunger is fully retracted. Without allowing
the cartridge to open, slide the tip and nosecone into the slot of the injector.
12. Immediate insertion is best. Allowing the loaded injector to dry out for
several minutes can encourage lens or optic capture and a torn IOL upon delivery.
13. I prefer not to fill the capsular bag with an OVD, but rather place a small
bolus of Healon5 into the center of the capsular opening. In this manner the
unfolding of the IOL can occur unimpeded under the bolus of Healon5 and drop
directly into the capsular bag. The bolus of Healon5 acts to push the IOL into
position and by remaining on top of the lens optic protects the corneal endothelium
while facilitating the OVD removal at the end of the case. This avoids the need
to rock and roll or tilt the IOL in order to remove the OVD trapped behind the
optic.
14. Position the injector tip bevel down and pass it through the incision such
that the tip overlies the center of the capsular opening.
15. Advance the plunger while directly visualizing the passage of the IOL and
haptics down the injector cartridge. Do not back up the plunger while advancing
the lens as this may override the optic or haptic causing an optic tear.
16. As the IOL unfolds, the leading haptic will position itself down and to
the left of the injector tip. Slightly rotate the barrel of the injector counterclockwise
900 to facilitate the remaining unfolding process.
17. Once the IOL has unfolded, and the trailing haptic is freed from the injector
barrel (and not before!) rotate the cartridge barrel to point the tip bevel
down. Retract the plunger making sure it does not capture the trailing haptic
as it does so, and use it as a positioning tool to engage and place the trailing
haptic into the capsular bag. Alternatively, if the trailing haptic fails to
release, use a forceps in the nondominant hand to remove the haptic and manually
position it into the bag. This is the most common stumbling block for
surgeons inexperienced with this lens insertion to experience. A little patience
here, pays off.
18. It is not necessary to position the haptics in any preferred orientation
so dialing the lens or moving it after it is implanted is best avoided once
the lens is in place.
19. Remember all good practitioners clean up after themselves. Never leave an
OVD in the eye at the conclusion of surgery anymore than you would leave an
IOL forceps. Visualize the complete irrigation and aspiration of any remaining
OVD from in front of, adjacent to, or behind the lens. A slight malpositioning
of the Tecnis optic is the telltale sign that there is trapped OVD. Once the
remaining OVD is removed, this IOL will self center without help.
Adopting the technology of the Tecnis modified prolate IOL into your practice
will more than reward the perseverant surgeon with better cataract surgery outcomes
and happier patients. The technology is here today and it is easier than ever
before to adopt into your practice. A new standard in surgical technology awaits,
shouldn’t you join in?
Robert M. Kershner, MD, MS, FACS is director of Eye Laser Consulting in
Boston, Massachusetts. He holds no financial or proprietary interest in any
product or company. Dr. Kershner can be reached at Kershner@EyeLaserCenter.com
References.
1. Kershner, RM. "Retinal Image Contrast and Functional Visual Performance
with Aspheric, Silicone, and Acrylic Intraocular Lenses-Prospective Evaluation
” Journal of Cataract and Refractive Surgery, September 2003; 29:1684-1694.
2. Tecnis IOL Package Insert 2004.
Figures.

The Tecnis IOL is a three-piece silicone lens
with a modified prolate anterior surface.

The IOL is loaded into the injection cartridge with the haptics at the two and eight o'clock positions.
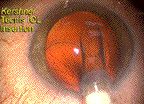
The Tecnis IOL unloads in a controlled fashion into the capsular bag with the leading haptic positioning down and to the left of the cartridge tip.
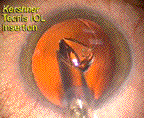
The optic begins to exit the cartridge

The optic gently unfolds into the capsular bag
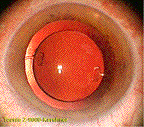
The IOL in position.